Hospitals up and down the country are encountering privatisation in various ways and to varying degrees. Reductions in hospital beds and services is leading to more NHS patients being referred to private hospitals for treatment, costing the NHS £1 billion in 2017/18
Not only this, the number of patients electing for private care and treatment is increasing, as a result of increased waiting times or restrictions to services due to rationing and spending cuts.
Private companies are procuring contracts for non-clinical aspects of hospitals as well, taking over the management of facilities and car parks - a contentious issue as ParkingEye, one of the largest private hospital parking management firms, made a £9.8m pre-tax profit last year.
Following the Health and Social Care Act in 2012, the amount of income that NHS hospitals were allowed to make from private sources increased to a 49% cap. This was a monumental increase from the previous 2% cap prior to this.
NHS PATIENTS REFERRED TO PRIVATE HOSPITALS
The number of NHS patients being treated in private hospitals has increased significantly over recent years. In 2015, 5% of NHS funded elective surgical admissions were to independent sector facilities, compared to just 0.35% in 2004/05.
The BMA report on these figures found it concerning that despite this growing role of private hospitals in NHS provision there continues to be no obligation for independent sector providers (ISPs) to report patient safety incidents and performance data.
NHS Improvement figures show that in the last two years over £1 billion has been spent by NHS trusts across England on buying health care from non-NHS bodies.
The number of patients being referred to private hospitals has reportedly surged by 600% in the last decades. NHS bosses describe it as a "last resort" option, where cancelling treatment would be the only alternative.
The most common treatment patients are being sent to private hospitals for are hip and knee surgeries, which is unsurprising due to the rationing and cuts these treatments have faced in recent years.
Phillippa Hentsch, of NHS Providers, said: “Hospitals have to hand over the patients because they have simply not got the beds, staff or theatres free to see them due to the pressures on the emergency side.”
WHAT IS CAUSING THE INCREASE IN REFERRALS TO PRIVATE HOSPITALS?
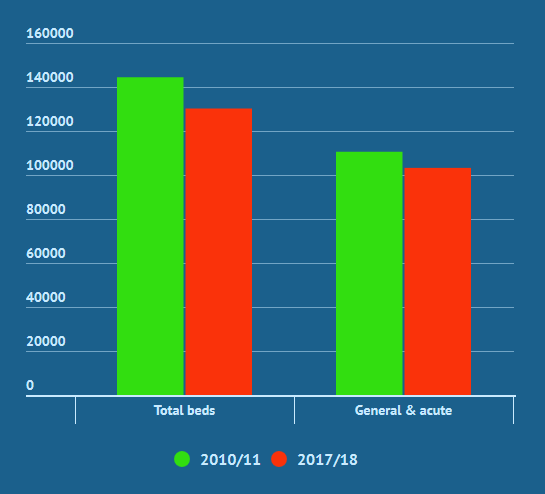
Data we compiled from NHS Digital shows that the total number of NHS beds available in England decreased by 9.85% between 2010/11 and 2017/11, down to 130,232. This is despite the number of admissions to hospitals increasing on average by 11% across England.
These figures come at the same time that the number of money being spent on sourcing care for NHS patients from private providers soars. With lack of beds, staff and resources to provide treatment many NHS trusts are having to pay more money to have the patients treated at private healthcare facilities.
It was reported in March 2017 that £901 million of the cash that had been earmarked for front-line services by the Chancellor was in fact was used to buy care from private or other non-NHS providers.
A Health Foundation report found that £1 in every £8 spent of local commissioners budget is on non-NHS provided care. This trend continued into 2017/18 as it was reported the figure of spending increased to £1 billion.
PATIENT SAFETY ISSUES IN PRIVATE HOSPITALS
With the increasing outsourcing of NHS patients to private hospitals for elective treatment, the issue of patient safety has been investigated by the Centre for Health and the Public Interest (CHPI).
500,000 patients are now treated each year in private hospitals across England. CHPI address some of the systemic patient safety issues in private hospitals. These include:
- Post-operative care in private hospitals is usually carried out by inexperienced junior doctors who are working excessively long hours.
- The consultant who carries out the surgery and who is responsible for the patient is permitted to be off-site.
- Nature of this post-operative care has been cited as a factor in a number of patient deaths.
- Lack of intensive care facilities means if something goes wrong then patients have to be transferred back to NHS hospitals, which in itself is very dangerous.
- Data on patient safety in private hospitals is poor and they aren’t required to make this information public in the same way as NHS hospitals are.
With the number of patients being treated in these hospitals increasing, particularly with the Choose and Book system or with acute trusts referring patients to clear extensive waiting lists, it is important to note these issues.
CHPI conclude that NHS commissioners and clinicians would find it difficult to avoid blame, and possible legal consequences, if NHS patients are harmed in private hospitals. Particularly now that the risks are openly documented.
This raises the issue of the cost of these referrals, both in the short term and the long term. In the short term, the cost of treatment for NHS patients in private hospitals is much higher than it would be if they could be treated in NHS facilities. Moreover, if something is to go wrong and there are legal consequences then it is the NHS that may have to pick up the bill in the long term.
In another report, the CHPI also document the safety issues in private hospitals following the scandal whereby surgeon Ian Paterson wounded 500 women who underwent unnecessary breast surgery in private hospitals. They conclude that until the private hospitals have full liability for the patients under their care, then there will be no guarantee of safety.
INCREASING USE OF SELF-PAY OPTIONS
A BMJ investigation has discovered that nearly 1,700 requests for hip and knee surgeries on the NHS were rejected in 2017-18. This is a 45% increase on the previous year. This comes following decisions made by many CCGs in recent years to limit the number of treatments to bring down costs.
GPs are now having to make more exceptional circumstances requests to try and obtain treatment for patients, more of which now are being turned down leaving patients in pain or turning to private treatment.
Ian Eardley, senior vice president of the Royal College of Surgeons, said, “The use of funding requests means patients will spend more time in pain with potential deterioration of their condition, thereby generating further costs for a system already under acute financial strain.”
More evidence is emerging that patients are deciding to pay for private treatment for hip and knee replacements due to NHS restrictions and longer waiting times.
Spire Healthcare saw a 12% rise in revenue from self paying patients in 2017. Certain areas have seen a particularly high surge in patients paying for care. Spire Little Aston Hospital, in the West Midlands, reported a 60% growth in patients paying for orthopaedic procedures in 2017. They said that some of this demand was driven by lengthening NHS waiting lists.
The Guardian reported in 2017 that patients without insurance can pay up to £14,880 for operations such as a hip or knee replacement or cataract removal. Profit-driven hospital firms are experiencing 15 to 25% year-on-year rises in the number of uninsured “self-payers”.
PRIVATE CARE WITHIN NHS HOSPITALS
Before the introduction of the Health and Social Care Act in 2012, hospitals were only permitted to make 2% of their income from private sources. However, when the legislation passed this cap was lifted to 49%.
The Independent probed an investigation into the effects of this change. Hospitals can now make considerably more money from private paying patients within the NHS institutions. For example, income from private patients for the Royal Marsden in London, a world-leading centre for cancer, increased by 105% from 2010/11 to 2016/17 up to £91.9 million. This made up nearly a third of its total funds.
Figures released quietly by the government acknowledged that the NHS in England made nearly £584 million from private patients in 2016/17, a nearly 29% increase from 2011/12.
The concerns with this are that a two-tier system is being created within the NHS whereby profits gained within NHS hospitals are going to American healthcare centres.
Moreover, these private patients are being treated by NHS doctors in NHS beds so private patients looking for world class facilities are using beds and services that should be provided by the NHS to our whole population.
Dr David Wrigley, a GP in Carnforth, north Lancashire said: “The fact private patients can jump the queue for treatment flies in the face of the founding ethos of the NHS – that all patients are seen as equal and treated according to need and not the ability to pay.”
A TWO-TIER SYSTEM?
The creeping privatisation within NHS hospitals, through the outsourcing of treatments and the increasing amount of money being made through private patients within NHS facilities, creates concerns of the creation of a two-tier healthcare system.
The Health and Social Care Act in 2012 paved the way for the eventual introduction of Accountable Care Organisations, or now rebranded ‘Integrated Care’ following controversy surrounding the similarities with the American healthcare system.
With specialist, world-leading hospitals such as Royal Marsden and Great Ormond Street able to make more money from private paying patients it takes away that specialist care from those unable to afford to jump the queue.
Following the change in law that allowed a cap on private patients in NHS hospitals increasing to 49%, Professor Allyson Pollock, director of Newcastle University’s Institute of Health and Society, said it has paved the way for the part-privatisation of the health service.
She said: “It’s not a surprise to see foundation trusts with niche specialities like cancer or cardiac [care] are turning to private patients.
“The problem is formerly these hospitals were almost 100 per cent public. Up to 49 per cent of the capacity – doctors, nurses and beds – can be diverted to private patients. In London … some of these patients will be very wealthy, medical tourists.
“The NHS is being squeezed and inevitably there will be a diversion of funds [from ordinary NHS patients to private ones].”