The NHS was set up to be a universal health service, covering the whole population, providing care according to clinical need, not ability to pay, and funded from general taxation.
Resources have never matched the level of demand for care, and there has always been a waiting list for some forms of treatment. This has fed the illusion that by paying for private treatment those with the fattest wallets can somehow ease the burden on the NHS and reduce the waiting lists; in reality this approach does not reflect how the resources available are shared between the NHS and the private sector.
A finite pool of staff
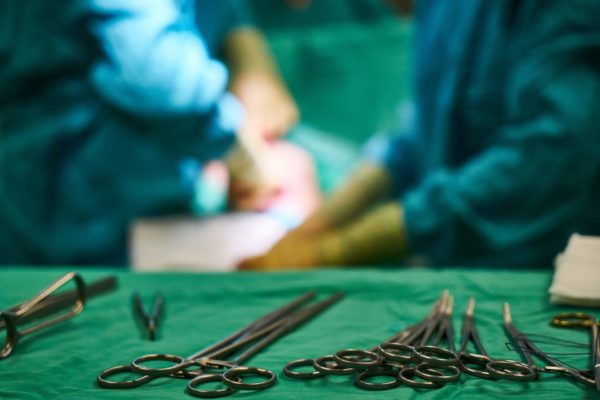
The majority of private hospitals employ doctors, surgeons and anaesthetists who also hold NHS posts. So if surgery increases in the private sector, it reduces staff availability for NHS work. In the case of other staff, such as nurses and allied health professionals, any increase in the scale and scope of the private sector means it makes a greater call upon the limited pool of staff available, and if the staff go to the private sector the capacity of the NHS is then restricted.
It should be noted that this pool of staff has, in the main, had its training organised and paid for by the NHS. For example, consultants are employed by private hospitals on a self-employed basis and the companies contribute nothing to their training.
Full article in The Lowdown, 21 June 2023